Returning to our home early Thursday afternoon, 33 hours post-delivery, was surreal. Most significantly (and obviously), while we had left our house just the two of us the day prior, we returned as a threesome. But it also felt like we were returning to a home that belonged in an alternative universe, where John’s strict maintenance of superficial order fell by the wayside. Laundry was literally strewn in every corner of our front living room. Amniotic fluid-soaked clothes were left in a heap in the bathroom sink. And, on our coffee table, John found a piece of paper with a series of times listed: 3:21am; 3:24am; 3:25am; 3:28am; 3:30am; 3:31, 3:34am; 3:36am; 3:37am; 3:39am; 3:40am; 3:41am. I had circled the last in the series, indicating it as the time my water broke. John picked up the paper and pointed to the list: “This. This is evidence of your insanity!”
* * * * *
I remember the day our daughter was born, one of the best days of our lives, in flashes, the majority of which are absolutely comical; some of which are altogether terrifying.
John will argue that I was likely in early labor most of the 16th. Having never been in labor, I assumed that the irregular tightenings in my lower abdomen were pre-labor contractions, which could begin days to weeks prior to the real thing. They didn’t stop me in my tracks, radiate, or worsen with movement. I think we tried timing them once or twice but gave up when we didn’t detect a pattern. Still, we were optimistic that maybe these “pre-labor” contractions were an indication that I would go into labor shortly, so John did not hesitate to accommodate one last craving for grilled cheese sandwiches and soup for dinner. He tried to persuade me to wash the food down with shots of hot sauce to encourage labor. We watched the presidential debates, I passed out on the couch, and John put me to bed at 11:30pm.
Around 1am I woke up with cramping and a need to use the bathroom. At 39 weeks, 6 days gestation and with 30 lbs of extra matter pressing on my bladder, these wake-ups were not unusual. I was a little surprised when I also had a bowel movement, but thought nothing of it. At 1:15am, the same thing happened. At 1:30am, I got suspicious, but I tried to go back to sleep, thinking that I would need my rest if I was going to be in labor for the next 15+ hours. Not possible. John was scheduled to work at 7am, so I thought I would let him sleep, since it still might be a false alarm.
I had a softly planned phone date with one of my closest friends that I had missed the previous evening. She lives in Alaska. At 2:10am EST (10:10pm her time) I texted: “Long shot, I know, but are you up now?” I listened as she told me about her recent romance over her birthday weekend, until the tightening felt like something I actually had to breathe through….weird. She was patient with me; she helped me time them, just 9 minutes apart. When it felt like I had three back-to-back, without much of a break, I tried to sound calm: “I love you, but I’m not really paying attention to you anymore. Call back later?”
The three contraction-like sensations in a row got me a little scared. Already this was not going right. Isn’t there supposed to be a slow ramp up? What am I supposed to do, now? If this was still prelabor bullshit, I thought I should take a shower; I had read somewhere that the warm water can help settle things down. It did not, but at least I was clean (not that it made a difference an hour later).
Next up: eat something. I would need my energy. I took a few spoonfuls of the soup from the evening prior before deciding that it was entirely unappetizing. Coconut water? Revolting.
It was about 3:00am, and I thought I was going to be seriously ill. I trudged my big belly to the bathroom upstairs, debating whether or not to try to have another bowel movement or vomit, or do both simultaneously. Opting to try the former, I saw a pool of blood collecting in the toilet—guess the “bloody show” I had read about was not subtle.
So now I thought things might be happening. I took out a piece of paper, a pen, and my cell phone, and I started writing down times: 3:21am; 3:24am; 3:25am…between each I noticed that I couldn’t stop shaking and, though the piercing sensation in my abdomen would lessen, the new radiating pain in my back would not. In a last-ditch effort to quell these “prelabor” contractions, I lay down on my left side on a plastic trash bag I had placed on the couch, just in case. And that’s when I felt what I can only describe as how you might imagine the unvocalized “POP” one makes when releasing pursed lips would feel. Although the rupture of membranes (my water breaking) was painless, almost pleasant even as I felt a momentary release of pressure, what immediately followed was not.
Get off the couch, get off the couch, get off the couch, I coached myself as I struggled to swing my legs under my weight. It took me three more contractions to make it back up the stairs, cursing the fact that both bathroom and the still slumbering husband were located a fourteen-foot climb away. I ripped off my soaked clothing and threw them into the bathroom sink, then trudged to the bedroom. Half-naked, I hunched over the foot of the bed. “John…”
“What’s going on?”
And here’s the part he will never let me live down: “I need help…timing contractions.” It wasn’t my intention to leave things out; I honestly just thought about what I acutely needed in that moment.
It was now slightly past 4am. I got into the only position that seemed tolerable: all fours, elbows and forearms on the ground, my right hand gripping my left fist. I would arch my back slightly with each contraction, which felt all-consuming at this point. I seemed to get little reprieve in between, not enough time to catch my breath before being slammed with the next. After a few of these, John concluded: “Okay, they’re about 90 seconds apart. So I’ll go take a shower.” (We don’t remember when John found out that my water broke, but he called to inform the midwife on-call, who told us to come on in, before he got in the shower.)
I think I was in too much shock to argue with him, and I still convinced myself that I would be in labor for a long time. I wanted to wait as long as I could before going to the hospital, to do everything I could to avoid being sent home because I wasn’t far enough along.
I don’t know how I got back up the stairs to finish packing my hospital bag while John was taking what had to have been the longest shower in history, I just know I didn’t get far. I so clearly remember being in the upstairs hallway, a few feet from our bedroom, gripping the bannister with all my will because I thought I was going to lose it. Things seemed to escalate in the blink of an eye and suddenly I was on my knees, feeling literally crippled. And I wanted to push…I needed to push. Shit!!
As I crawled to the bathroom where John was showering, my first thought was, String of expletives!! If this is early labor, there is no way I can do this! My second thought: This is not like the early labor I’ve seen. Oh God, something might be seriously wrong. I made it to the bathroom: “John, I feel like I need to push…”
I heard the water turn off immediately, and then, “Don’t!” He hurried out and got dressed, while I took a quick look at myself in the mirror for I have no idea what reason…I was bracing myself against the bathroom sink, and the mirror was there. It was cold and I was standing there in nothing but a cotton nightgown, beads of sweat coating my upper lip and forehead. John threw a few more things into the suitcase and I aimlessly tore through a pile of clean laundry, looking for cloths I could wear later. “Anna, just get in the car, and don’t push!” (He would later tell me that watching me walk to the car was like watching someone walk on eggshells.)
I thought it would be impossible to sit. I managed to get into the car, putting as much weight as I could on my toes and shoulders, raising my butt and thighs up as though the seat was on fire. I fastened my seatbelt, but I gripped it with both hands, holding it away from my body; its touch was simply too much stimulation.
John threw bags into the car, got in, and started driving quickly. He coached me to take short, percussed breaths, as though I was blowing out a candle. As we were stopped at a stoplight, a contraction momentarily lessened and I glanced at the dashboard clock: 4:57am. My thoughts: Oh God, shit’s going to get a lot worse again when it hits 4:58.
We got to the hospital at about 5:10am. John initially drove past the hospital in search of parking. All I needed to do was glance sideways at him; he floored it in reverse back to the hospital entrance and parked in a tow-away zone.
John was a few steps behind me as I approached the security guard. He tried to drape a bathrobe over my shoulders. I flung it off. (I might have also barked, “Don’t touch me!” Opinions vary.) The security guard did not argue when I refused the wheelchair or any assistance. I had done my Ob/Gyn rotation at the hospital; I knew the quickest way to get to the PETU (the Perinatal Evaluation and Treatment Unit, where women in labor are evaluated prior to admission), and I’d be damned if I had to wait for a wheelchair (that and I didn’t know how I would possibly sit in one).
I became more nervous as I approached the nurses at the front desk of the PETU. During my time on Labor and Delivery, every woman I saw come in got initially sent to the waiting room, and I knew I would just go crazy if I was asked to wait for hours. As I introduced myself in fractured phrases, bracing myself against the desk (the nurses vaguely remembered me from my rotation), I was surprised by how much attention the nurses seemed to be giving me. One interrupted: “You can go ahead in exam room 2 and the doctor will be 30 seconds behind you.” Seriously?!! Awesome!
I remember getting to the bed and John helping me out of my nightgown and into a hospital gown. (I had thought about staying in my nightgown, but it was soaked with amniotic fluid and perspiration.) As the nurse promised, the resident was in the room before I finished putting the gown on. The cervical exam—when the physician/midwife/nurse checks to determine dilation (you need to be 10cm to deliver), effacement (the thinning of the cervix, 100% to deliver), and station (the degree of engagement, or how far the baby’s head has descended into the pelvis)—was remarkably fast. She barely inserted the tips of her first two fingers before drawing back, “You’re complete. Well done.”
Complete? Completely what? “Dilated?” I asked, shocked.
“Yeah! Go ahead and start pushing!”
I was so relieved that I wasn’t in early labor—it all started to come together. That horrible mixture of nausea, pain, and a need to push that began in our upstairs hallway was likely transition, the dreaded limbo period between active labor and the pushing part. Thank God I could now start pushing!
And then, I had another thought, “So, no epidural?”
The resident laughed, “No way!”
“Nubain?” (Another pain-relieving drug sometimes used to take the edge off during labor and delivery.)
“No time,” replied the resident. “You’ll have this baby out before the drug can take effect.”
I had wanted to try laboring without pain meds, and now I didn’t have a choice. It was funny how quickly my mind shifted. The fear I felt at home dropped away. I would deliver this baby because I had no other option.
I was allowed to push and scream my bloody head off as they wheeled me from the PETU to Labor and Delivery. In between contractions, one of the nurses asked John and me what in med school is called an AMPLE history (basically, what you need to know about a patient in an urgent setting: Allergies; Medication; significant Past medical history; Last oral intake; and Everything else).
It came out that I was allergic to ferric gluconate, an iron infusion that I had once been given when I was quite anemic. So of course that raised concerns—no one likes the thought of a woman predisposed to having a low red blood cell count losing a ton of blood during delivery, therefore collapsing her veins and making IV placement nearly impossible post-delivery. The nurse explained that she wanted to place a hep-lock (a small tube connected to a catheter in a vein to allow for easy IV access). I could not fathom getting an IV placed while I writhed with each contraction. I started to protest, but John quickly convinced me to just let her try, reminding me that it was just a hep-lock, just a way to gain access should they need to later. She must have placed it mid-contraction; I didn’t notice it.
As soon as we got to the delivery room, they shifted me into the bed and collapsed the bottom part down—go time! Sue, the midwife on call, introduced herself and her midwifery student, Hannah. She wore a visor over her face and I remember her looking calm. She instructed the nurse on my left and John to each grab a leg, and she told me to let her know when I wanted to push, and then push as hard as I could on her count of ten.
Later that day, John would tell me that he now understood why some men have a vasovagal response (a feeling of sudden light-headedness with a possible faint in response to a trigger) during delivery. He had never heard such a bloodcurdling scream produced by a loved one. At one point the nurse holding my left leg said something to the effect of, “You could produce more effective pushes if you didn’t scream so much and redirected some of the energy…” I could see John in my peripheral vision smile slightly and pinch the bridge of his nose as if to say, “Oh damn! Anna’s going to rip her a new one!” I didn’t have time or energy to think of a snappy retort, instead I “redirected” some of my pissed-offedness into the next contraction.
Frustrated by the uneven force exerted against my legs, I asked if I could use the squat bar. John didn’t hold back, “No, you can’t! Are you crazy?! You’re going to have this kid out in like three pushes!” Then he turned to Sue and back to me, “Oh, sorry, probably not my place to say anything.”
To which Sue replied, “Eh, it’s probably better coming from you.”
“Yeah…I don’t think so.”
One of the things I appreciated immediately about Sue was her ability to calmly explain things clearly and succinctly. She went on, “Anna, you’re almost done. You will deliver this baby in the next few pushes.”
I looked at her skeptically, “Are you shitting me?!” I kept thinking that maybe everyone was telling me we were so close as a kind of motivation, when really it could be another couple hours.
She laughed. “I’m not. Do you want to feel the head?”
John guided my hand. As I felt the top of her head, I was again overcome with a feeling of have to. The word can didn’t enter my thought process; I was not motivated by a sense of ability, but a feeling that I didn’t have a choice.
I felt a wave of release as her head was delivered. I had been scared about delivering the shoulders, as they seemed objectively wider and sharper than the head. But they somehow managed to just slide out with the next push, with I’m sure help from Hannah, the midwifery student who I only then noticed had been the one at the helm. She applied downward pressure so that the anteriorly placed left shoulder could pop out first, then the right.
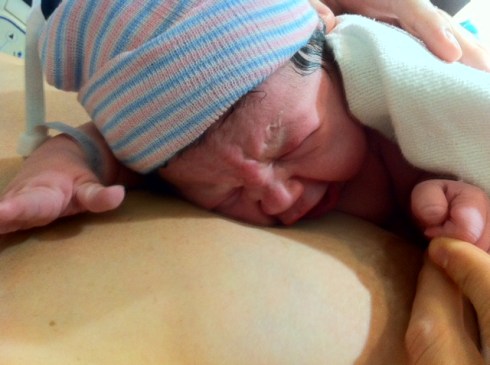
A split second later, my wailing girl was placed on my belly, and I instantaneously started crying myself. John so clearly shared my simultaneous joy and relief, an intensity neither of us had ever experienced! A screaming, pink newborn moving all her extremities—in her first second of life, she gave us so many indicators that she was doing well! (Though, as you can see below, she looked a bit like “a Kracken from the sea!”–John calls these the “put me back in!” pictures :)) It was 5:43am.
Now the next part that had me irrationally terrified: the delivery of the placenta. It’s normally a comparatively easy process, but I had seen one instance of a retained placenta, where a woman had to go under general anesthesia to have it removed. But I remember no details about the delivery of the placenta, that’s how insignificant it was.
Meanwhile, Aurelia blew me away from minute one of life! She lifted up her head and used her arms to rake her way up to the breast. Instinctively, I tried to help her by holding her under her arms, but this was before the placenta was delivered, and Sue cautioned me not to pull on her while the umbilical cord was still pulsating.
After the placenta was delivered, John cut the cord and Aurelia raked the remainder of the way to her food supply. She latched and started suckling, but took a break for a quick photo op.
While Ari ate away (well, attempted to), Sue explained that she wanted to give me a shot of Pitocin in order to prevent postpartum hemorrhage, which is more common in abnormally quick deliveries. Fine. And it could be given through the hep-lock that was already in place, so I even avoided a needle stick.
Meanwhile, Sue and Hannah checked me for tearing. They found both posterior (toward the rectum, common) and anterior (toward the urethra, relatively uncommon) lacerations, second degree (the lacerations extended into the muscle but not into the rectal sphincter . John and I were both surprised. He assumed that, with the speed of my delivery, my lacerations would be more severe. I honestly didn’t feel ripping during the delivery, so I thought any lacerations would be superficial, if present at all.
Sue told me that in order to protect my urethra, she wanted to place a catheter during the repair. No question. I was nervous, because I had had a urinary catheter placed before and the process was…uncomfortable. But my desire to urinate normally in the future trumped temporary discomfort. Plus I had just delivered a baby, so how terrible could it be?
Before they started the repair, I interjected, “Wait, I get Lidocaine for this, right?”
“Oh God yes,” Sue responded. “As much as you need.” And then she proceeded with the Lidocaine injection into my labia, “Small stick, and then you’ll feel some numbness in a few seconds.”
With my permission, Hannah took a try at the repair first, but Sue took over in places, as anterior lacerations are a little tricky and not something about which you want to be cavalier. I was shaking and my teeth were chattering uncontrollably, in part a side effect of the Pitocin. The nurse who had previously (in my mind stupidly) told me to stop screaming so much, kept layering on the warm blankets, for which I was grateful. And of course we had Ari to distract us. There were moments when I felt the sharp slice and pull of the needle, but then they would administer more Lidocaine and all was well.
Oh shit! I thought suddenly. “John, the car!” It was still parked illegally at the entrance of the hospital. “You have to go move it.”
“Woman, you crazy! I’m not leaving now.” If we got towed, it would just make for a good story.
The repair took almost 90 minutes. It included a lot of gentle coaxing, “I know it’s hard, but try to relax your knees.” I wanted to, but I could not stop shaking. All the while Ari was trying to figure out this feeding through mouth thing. But I was happy for them to take their time so all my parts would be as close to pre-delivery as possible.
After the repair, while the nurses were cleaning me up and Ari was temporarily taken to be cleaned and warmed, I was able to convince John to go move the car if for no other reason than I wanted some of my own clothes to wear. When he returned (the car had miraculously not been towed!), a nurse was helping me out of bed and into a wheelchair for transport to a postpartum room. I could not believe that I could get up and walk (a short distance) on my own!
There must have been a lot of folks banging in January because the postpartum floor was packed! I was assigned a double room to share with another mother, which I didn’t mind except that it meant John couldn’t stay the night with me. (We were lucky to have a good friend live a few blocks away who generously offered John a bed.) After we got settled—which took a few minutes due to being off-kilter from the immediate loss of 20+ pounds of baby + amniotic fluid + blood, and the passing of gulf ball-sized clots (I kid you not)—we anxiously awaked Ari’s return. Every time we heard the door open, we would search for her.
My heart melted when they brought her. I know they say that the love you feel for your child is instantaneous and beyond measure, but when she was returned to us, I felt like I had a better grasp of and appreciation for it. She came into this world like a bat out of hell; I felt scared, and also distracted by the surroundings that I could suddenly focus on again: I realized that we were in the birthing suite; I saw who else was in the room; I felt the placement of the stiches sewing up my perineum. There was so much! Back in our recovery room, it was just we three.
Our day of recovery was a blur. I remember calling loved ones. I remember classmates and residents visiting. I remember taking an uncomfortable walk around the ward with my two loves. I remember many failed and successful attempts at nursing. I remember the fabulous sushi dinner (so much raw tuna!!) John brought in. I remember calling John at 10pm in tears, asking if I was allowed to go to sleep in case anything should happen to our daughter in the crib next to me. And I remember walking out of the hospital in my nightgown because, in the rush to get to the hospital, we had forgotten to pack things like pants and bras.
Driving home together before rush hour on a crisp, bright October day, I kept thinking: I cannot believe I get to keep her! She is ours and we are hers, always. And then the real fun began…







wow. just, wow. this actually made me cry. more than once. you are a wonderful writer 🙂
Thank you, Ellen! I’m really flattered you got through even a few paragraphs–I know it’s a lot It was good to re-remember it 🙂
It was good to re-remember it 🙂
Jeesh Anna, you made me cry. I’m still panting.
haha, thanks Dad!
Thank you so much for sharing your story. I am currently a second year medical student and expecting my first baby any day. I am 39weeks 1 day and feel like he will never come. I am also trying to figure out life and studying for step one and reading your story this morning was just what I needed. I am having that end of pregnancy anxiety on top of will I be able to pull off boards in July. It is easy to be so focused as a medical student on so many details and reading your story I could feel the joy coming off the page, it gave me a little bit of renewed calm and reminded me how exciting this time is for me. Thank you.
Hi Jamie! Congratulations!!! I’m so happy for you! Oy! 39 weeks, 1 day–I remember the feeling all too clearly. I loved being pregnant, for the most part, but I had had enough come 37 weeks. And you’re having a little boy? That’s wonderful!
I have to admit, I am terrible at getting anything done while at home–but some women and men are much better at this (and some babies are also more accommodating). You will certainly figure out something that works for you. And if you have to miss some time with him while you’re studying, it’s not as though the months 5-6 are any less precious than 1-4…just take what you can get, and try not to worry about what you’re not doing (not that I am ever one to give advice, and I know it’s easier said than done…but it’s kind of my regret of the first two months). This is a wonderful time, and I wish you the best of luck on your delivery.
Thank you so much for your kind words!
Anna, thanks for sharing your experience. It’s funny how everything is so confusing and uncertain when you’re in the middle of it and so obvious in hindsight, isn’t it? I really loved your honest responses and outbursts. With my first, I let Chris sleep when I was having contractions for about 2.5 hours while I was trying to “figure out” whether or not my water had actually broken the night before (I had the little drip, not the big gush) and if my contractions were, in fact, regular or if I was just being delusional at 3am. So it’s not just you 🙂 I still haven’t gotten around to writing down either of my birth stories, although I think about doing it all the time. You’ll be amazed how many little details (especially bad ones) just seem to somehow seep out of your memory even just 6 or 12 months later so you’ll be happy you have this written out one day. I can’t wait to meet your little family in person. Maybe this summer?
Thank you so much for your sweet words, Tina. I would LOVE to hear your birth story…and I would love to meet your little ones, of course! I take the boards in July, but I should be in VA a ton in August, if you’re around.
I also thought I was delusional about my contractions, even while I was writing them down…just didn’t make sense!
And, yes, I hear you about forgetting the bad details…in my case, they were mostly just normal pain. I forget so much…and then John and I make love and I remember at least part of the pain. (My midwife said that the lacerations normally take six months to fully heal?)
And aren’t we both so sweet to let our hubbies sleep? 🙂 xoxo
Love this! It’s my dream to have a quick labor someday – one like yours where they check and you’re ready to go! Not there yet, but maybe on like, our 5th or 6th baby 😛
hahaha! but didn’t you, like, vomit a baby out this time? doesn’t seem pleasant, but it doesn’t seem ridiculously slow either 🙂 (come to think of it…I forgot the moment when I started retching at the hospital, they tried to put an emesis basin at my face, and I had to push it away because I preferred vomiting all over myself than have anything touch me!)
i feel poorly ever complaining about the terrifying and painful moments during my delivery, because i know i had it good…maybe a reward for having a tough time getting pregnant?
i’m sure number 5 or 6 will practically walk out of you. you rule!
Thank you so much for sharing your birth story Anna. Your little lady is gorgeous.
Thank you so much, Stephanie! I hope you’re well!
love you, Anna! thanks for sharing 🙂
love you back! so excited to meet your little girl!
Hey Anna, I just now had a chance to read your birth story. It was wonderful! You’re a great writer, not to mention a wonderful mother and wife. Hope all three of you are doing well.
Thank you so much, Krystyna–that’s so kind of you! Much love to you and your hubby 🙂
I just wanted to say thank you. Every birth story is different, but there were many similarities between ours. Waking in the middle of the night, not really sure what was happening, husbands who want showers (and in my case, wanting to clean the shower just in case we had relatives come to stay)… Your medical knowledge adds a layer of understanding for those of us who have experienced birth but don’t really know all the technical terms. So what I’m trying to say is Thank You for inspiring me to write my own birth story!
Hi Sue! Thank you for your comments. I think I would have gone out of my mind if John tried to *clean *the shower–jeez! And I’m touched that you’re thinking of writing your own birth story after having read mine; I enjoyed the process more than I had anticipated 🙂 Thank you again!
This brings back my four childbirth experiences as if they had happened only last year! Thanks so much!